Medicaid PPP New Jersey
At Home Health Ameri Care , High-quality, affordable home care services for improved quality of life and peace of mind.
Medicaid PPP Program
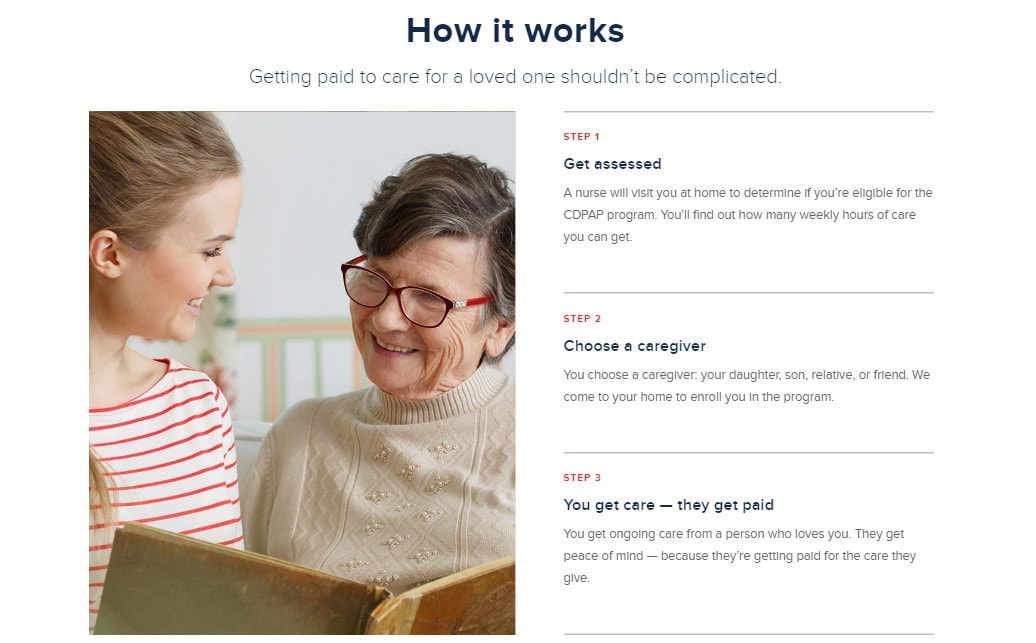
- New Jersey Department of Human Services Division of Medical Assistance and Health Services Personal Preference Program
- Recognizing the needs and preferences of many of the state’s seniors, New Jersey’s Medicaid program offers the Personal Preference Program (PPP). The PPP provides financial assistance to elderly and / or disabled, Medicaid-qualified residents to help them live independently and manage their activities of daily living.
Based on the “Cash and Counseling” model, the program distributes to participants a budget that would otherwise be spent on services for them. Participants have the power to select their own care providers. Program participants can hire friends and family members, so relatives, including spouses, can be paid to be caregivers if they are at least 18 years old. Program participants who are cognitively challenged or unable to direct their own care can still participate in the program, given they elect a representative to assist in making decisions on their behalf. The representative may be a friend or relative, but cannot also be the hired caregiver. A fiscal intermediary agency handles the financial responsibilities, such as processing payroll and deducting taxes.
This program and the category of programs are referred to by many different names. The Personal Preference Program might also be referred to as Personal Care Assistance (PCA) services. Cash and Counseling programs, in general, are also known as consumer direction, self-direction and participant-direction.
Benefits and Services PPP Program
The program includes both medical coverage and also home care and personal care services. Because state rules had previously restricted the number of qualified elderly Medicaid participants who could receive Home and Community Based Services, elders who wanted to receive their care outside of a nursing home often had to put their name on a waiting list. This is no longer the case.
In addition to the emergency and primary medical services that are provided through the Managed Care Organization, participating individuals in New Jersey may be able to receive these non-medical services:
In addition to the emergency and primary medical services that are provided through the Managed Care Organization, participating individuals in New Jersey may be able to receive these non-medical services:
- Adult day care
- Assisted living care / adult family care
- Behavioral health services
- Care management
- Home & auto modifications
- Home care
- Mental health / addiction services
- Nursing home care
- Personal assistance
- Personal Emergency Response Services (PERS)
- Prepared meals brought to the residence
- Respite Care
Eligibility Guidelines
Functional Need
Program candidates must have a need for assistance with their activities of daily living, such as bathing, toileting, and eating as determined by a healthcare professional. However, their needs cannot be so severe that full-time nursing home level care is required.
Financial Need
Candidates must be financially eligible for NJ Medicaid (FamilyCare) Plan A. These requirements vary depending on one's marital status and whether one's spouse is also applying.
Individuals Applying for Medicaid - In 2020, seniors can have up to $2,349 in monthly income ($28,188 annually). Persons over that limit may still qualify if they have excessively high medical expenses. This pathway to eligibility is often referred to as medically needy. That said, it’s important to note that the medically needy income limit is much lower than the abovementioned income limit. NJ also allows applicants who are over the gross monthly income limit to use a special type of account to ensure that they spend their excess income on medically necessary goods or services. Individual applicants can have countable assets valued at $2,000, which does not include the equity value of their home, up to $893,000.
Couples Applying for Medicaid - In 2020, married couples, with both spouses as applicants, can have up to $4,698 in monthly income, or put differently, each spouse can have as much as $2,349 / month in income. The couple can have $3,000 in countable assets. Their home and vehicle are non-countable assets and don't count towards the $3,000 limit. However, as previously mentioned, home equity valued at more than $893,000 is not considered exempt.
Couples with One Spouse Applying - Persons in this situation have considerably more flexibility when seeking Medicaid. In 2020, the non-applicant spouse can have up to $128,640 of the couple’s joint resources. (This is commonly called a community spouse resource allowance and is in addition to the $2,000 in assets the applicant spouse can retain). In addition, an applicant spouse’s income, up to $3,216 / month, can be allocated to the non-applicant to provide him or her with sufficient financial resources on which to live. (This is called a monthly maintenance needs allowance). This calculation includes accounting for local housing costs. Shifting income from the applicant spouse to the non-applicant spouse can also lower the applicant's income to the acceptable limit.
Program candidates must have a need for assistance with their activities of daily living, such as bathing, toileting, and eating as determined by a healthcare professional. However, their needs cannot be so severe that full-time nursing home level care is required.
Financial Need
Candidates must be financially eligible for NJ Medicaid (FamilyCare) Plan A. These requirements vary depending on one's marital status and whether one's spouse is also applying.
Individuals Applying for Medicaid - In 2020, seniors can have up to $2,349 in monthly income ($28,188 annually). Persons over that limit may still qualify if they have excessively high medical expenses. This pathway to eligibility is often referred to as medically needy. That said, it’s important to note that the medically needy income limit is much lower than the abovementioned income limit. NJ also allows applicants who are over the gross monthly income limit to use a special type of account to ensure that they spend their excess income on medically necessary goods or services. Individual applicants can have countable assets valued at $2,000, which does not include the equity value of their home, up to $893,000.
Couples Applying for Medicaid - In 2020, married couples, with both spouses as applicants, can have up to $4,698 in monthly income, or put differently, each spouse can have as much as $2,349 / month in income. The couple can have $3,000 in countable assets. Their home and vehicle are non-countable assets and don't count towards the $3,000 limit. However, as previously mentioned, home equity valued at more than $893,000 is not considered exempt.
Couples with One Spouse Applying - Persons in this situation have considerably more flexibility when seeking Medicaid. In 2020, the non-applicant spouse can have up to $128,640 of the couple’s joint resources. (This is commonly called a community spouse resource allowance and is in addition to the $2,000 in assets the applicant spouse can retain). In addition, an applicant spouse’s income, up to $3,216 / month, can be allocated to the non-applicant to provide him or her with sufficient financial resources on which to live. (This is called a monthly maintenance needs allowance). This calculation includes accounting for local housing costs. Shifting income from the applicant spouse to the non-applicant spouse can also lower the applicant's income to the acceptable limit.
FAQ PPP Program
What is the MEDICAID New Jersey Personal Preference Program (PPP)?
The New Jersey Personal Preference Program (PPP) offers an alternative way for NJ FamilyCare Plan A members to receive their Medicaid Personal Care Assistant (PCA) services without the use of a home health care agency. The PPP allows elderly and disabled Medicaid recipients to self-direct and manage their PCA services
What does “Self-Directing” mean?
Self-directing emphasizes independence and empowerment by expanding your degree of choice and control over your long term services and supports. It allows you and your authorized representative to serve as the employer and take responsibility for directly hiring, training, supervising, and firing your paid workers. You and your authorized representative become the experts on your own care and are able to determine the services and supports that best meet your personal care needs.
The PPP offers you greater control, flexibility, and freedom. You can choose who provides your care, what type of care you want and need, when you want care to be provided and where the care will be provided. Workers become accountable to you/authorized representative.
n self-directed programs, you negotiate PCA wage rates within the program rules, purchase other goods and services to increase safety and independence in the home or reduce your need for paid services. You may also choose to take 10% of the monthly budget as cash for justifiable purchases of goods and services not readily available through other means.
The PPP offers you greater control, flexibility, and freedom. You can choose who provides your care, what type of care you want and need, when you want care to be provided and where the care will be provided. Workers become accountable to you/authorized representative.
n self-directed programs, you negotiate PCA wage rates within the program rules, purchase other goods and services to increase safety and independence in the home or reduce your need for paid services. You may also choose to take 10% of the monthly budget as cash for justifiable purchases of goods and services not readily available through other means.
How do I qualify for the Personal Preference Program?
- Your Managed Care Organization must determine your eligibility for Medicaid PCA services;
- You must be NJ FamilyCare Plan A enrolled;
- You must require assistance with activities of daily living;
- You must be currently receiving or eligible for Medicaid PCA services from a home health agency;
- You must have the ability to direct and manage services, or elect an authorized representative that can assist you with the program
How does the Personal Preference Program work?
You or someone you designate as authorized representative can chose the workers you want to hire to provide your personal care services. You decide what schedule this person will follow, how much you pay them, and the job responsibilities they perform within your approved budget.
The PPP uses the hours of service authorized from the PCA assessment from your MCO to determine the monthly budget. The number of hours authorized is converted to a dollar amount using the reimbursement rate with a standard administrative deduction to cover counseling and bookkeeping services.
A financial consultant will assist you in developing a cash management plan to help determine how best to spend the monthly budget to meet your personal care needs.
The PPP uses the hours of service authorized from the PCA assessment from your MCO to determine the monthly budget. The number of hours authorized is converted to a dollar amount using the reimbursement rate with a standard administrative deduction to cover counseling and bookkeeping services.
A financial consultant will assist you in developing a cash management plan to help determine how best to spend the monthly budget to meet your personal care needs.
How does this program differ from the Medicaid Personal Care Assistant (PCA) Program?
The PPP differs from the PCA program in that it allows for more consumer control, flexibility, and direction. Instead of relying on an agency to provide the services, the PPP allows you to hire your own worker to handle your needs.
The PPP requires you to become an employer, which requires additional responsibilities. You will now be the employer of record.
The PPP requires you to become an employer, which requires additional responsibilities. You will now be the employer of record.
What are the benefits of participating in the Personal Preference Program?
- Decision making power is increased. Participation through the traditional agency delivered service model limits your control; however, self-directing provides more independence in directing your own care needs. Professional advice from your financial consultant is available to aide you in making your own informed decisions about the type of services necessary to meet your needs.
- Support of informal caregivers is increased. You may prefer to choose a family member or friend to assist you. The PPP allows these chosen individuals to be paid for this service. This could enable a relative to stay at home and care for a spouse, parent or child, and receive payment for their services.
- Appropriate and selective services. The PPP allows you and your family to decide what services are most appropriate
Who pays for this program? Will I have to pay any out of pocket expenses for participating?
Medicaid pays for the PPP. You do not have to pay anything related to participating in the PPP. However, your total budget is reduced each month to pay for the PPL administrative fee
Can out-of-state college students qualify for the Personal Preference Program?
Yes. Participants who are enrolled in a college/university on a full-time basis in/out of state are subject to the following:
• Participating student must be present at their New Jersey address to participate in home visits and nursing reassessments; and,
• Must provide documentation of progress towards completion of a planned educational goal, such as a degree, certification, accreditation, etc.
• Participating student must be present at their New Jersey address to participate in home visits and nursing reassessments; and,
• Must provide documentation of progress towards completion of a planned educational goal, such as a degree, certification, accreditation, etc.
Do individuals who have cognitive challenges have the opportunity to participate?
Yes. Individuals with cognitive challenges are eligible to participate as long as they have an authorized representative to help make decisions. The authorized representative may be a relative or close friend who is willing and able to assist the individual in planning for and purchasing care. *It is important to understand that the authorized representative cannot be the same person as the worker.
Can individuals who attend camp or a day program qualify for the Personal Preference Program?
Individuals attending camp can only receive services if the camp program does not provide PCA services. Individuals attending a day program may not receive Personal Preference services since PCA is the responsibility of the day program.
If I am unable to manage my services, would I be able to qualify?
If you are unable to manage the responsibilities of directing and supervising your personal care need you may participate, but will be required to have an authorized representative to act on your behalf. An authorized representative may be your legal guardian, a family member, or any other individual identified who willingly accepts the responsibility for decision-making on your behalf who must reside in New Jersey. An authorized representative must demonstrate a personal commitment to you, be willing to follow your wishes and respect your preferences while using sound judgment. The authorized representative receives no monetary compensation for this service and may not serve as your worker.
What is the role of the Fiscal Intermediary in the Personal Preference Program?
PCG Public Partnerships, LLC (PPL) is the fiscal intermediary (FI) contracted by the New Jersey Department of Human Services (DHS) to provide services for the Personal Preference Program.
PPL provides guidance regarding:
PPL provides guidance regarding:
- Your rights and responsibilities as an employer;
- Budgeting your cash management plan;
- Processing worker payroll; and,
- Making payments for any goods and services included in your monthly budget.
What can I purchase with my monthly budget?
• Employment of individuals, including family members, to provide personal assistance;
• Cleaning services from private companies to clean personal areas including bedroom, bathroom, kitchen, etc.;
• Errand service to assist with banking, shopping and other types of routine tasks;
• Laundry service from a laundromat or other provider; and,
• Supplies and equipment that promote or enhance independence that are not covered by Medicaid.
• Cleaning services from private companies to clean personal areas including bedroom, bathroom, kitchen, etc.;
• Errand service to assist with banking, shopping and other types of routine tasks;
• Laundry service from a laundromat or other provider; and,
• Supplies and equipment that promote or enhance independence that are not covered by Medicaid.
How is the monthly budget determined?
Your MCO (Aetna, Amerigroup, Horizon NJ Health, UnitedHealthcare Community Plan or WellCare) is responsible for authorizing the number of Medicaid PCA hours you are eligible to receive, to provide you with options counseling and to enroll you into the PPP.
The MCO uses the hours of service authorized from your initial PCA clinical assessment (or most recent reassessment) as the basis for determining your monthly budget. The number of authorized hours is converted into a dollar amount using the current reimbursement rate. A standard administrative deduction is then calculated to cover the costs of counseling and bookkeeping services. The remaining amount is available to you for purchasing services.
The financial consultant will assist you in developing a cash management plan to help determine how best to spend your monthly budget to purchase services that you need.
For example if a participant is eligible for 40 hours a week based on the MCO assessment, the participant’s budget is calculated like this:
Step 1. The number of hours awarded by the MCO is multiplied by the State’s reimbursement rate of $15 per hour. This includes cost and does not represent the rate of pay you must pay your worker per hour.
Step 2. Multiplied by 4.33 which is the calculation used to account for the different number of days in each month.
Step 3. Multiplied by the fiscal intermediary service fees at 12.5%.
Step 4. The participant has a monthly budget in the amount of $2,273.25
40 (Hrs. Awarded) X $15 (State’s Reimbursement Rate/Hr.) = $600
$600 X 4.33 (Monthly Calculation) = $2,598
$2,598 X 12.5% (FI Fees) = $324.75
$2,598 - $324.75 = $2,273.25 (Monthly Budget)
The MCO uses the hours of service authorized from your initial PCA clinical assessment (or most recent reassessment) as the basis for determining your monthly budget. The number of authorized hours is converted into a dollar amount using the current reimbursement rate. A standard administrative deduction is then calculated to cover the costs of counseling and bookkeeping services. The remaining amount is available to you for purchasing services.
The financial consultant will assist you in developing a cash management plan to help determine how best to spend your monthly budget to purchase services that you need.
For example if a participant is eligible for 40 hours a week based on the MCO assessment, the participant’s budget is calculated like this:
Step 1. The number of hours awarded by the MCO is multiplied by the State’s reimbursement rate of $15 per hour. This includes cost and does not represent the rate of pay you must pay your worker per hour.
Step 2. Multiplied by 4.33 which is the calculation used to account for the different number of days in each month.
Step 3. Multiplied by the fiscal intermediary service fees at 12.5%.
Step 4. The participant has a monthly budget in the amount of $2,273.25
40 (Hrs. Awarded) X $15 (State’s Reimbursement Rate/Hr.) = $600
$600 X 4.33 (Monthly Calculation) = $2,598
$2,598 X 12.5% (FI Fees) = $324.75
$2,598 - $324.75 = $2,273.25 (Monthly Budget)
How do I receive my monthly budget?
As the fiscal intermediary for the program, PPL issues the budget on a monthly basis. The monthly budget amount is deposited into an account established by PPL for you. You direct PPL to make payments through the use of your cash management plan, as you see fit. PPL handles all payroll responsibilities, tax deductions and withholding obligations.
What can I do if I disagree with the determination of hours assessed by my Managed Care Organization?
If you are not in agreement with the assessment determination you can call your MCO and ask for an appeal. You are entitled to an internal appeal with your MCO. If you are dissatisfied with the outcome of your internal appeal, you can file for a state fair hearing. There are timeframes you must follow with the internal appeals process and the fair hearing process. Your MCO will advise you of those timeframes and guide you through the process.
What happens if I overspend my monthly budget?
You or your authorized representative may not allow your worker(s) to work more hours than authorized by the monthly budget as specified in the cash management plan.
How does this monthly budget affect my personal income?
Supplemental Security Insurance Benefits:
Your Supplemental Security Insurance (SSI) benefits will not change because of your decision to participate in the PPP. Your monthly budget will not be counted as income or as a resource for SSI during your participation in this program. You may decide to disenroll from the PPP at any time. This decision will not affect your SSI benefits. However, any money left in your budget will be returned to the state. For more information regarding impact to SSI benefits for the household, please consult https://www.ssa.gov/.
Supplemental Nutrition Assistance Program Benefits:
Your PPP monthly budget is not counted as income or as a resource for your Supplemental Nutrition Assistance Program (SNAP) benefits (formerly known as food stamps). However, wages paid to your PPP worker do count as income for their SNAP eligibility. If you are in the same household as the person providing your care, it may affect the amount of SNAP benefits for the household. You may decide to disenroll from the PPP at any time. This decision will not affect your SNAP benefits. However, any money left in your budget will be returned to the state.
Your Supplemental Security Insurance (SSI) benefits will not change because of your decision to participate in the PPP. Your monthly budget will not be counted as income or as a resource for SSI during your participation in this program. You may decide to disenroll from the PPP at any time. This decision will not affect your SSI benefits. However, any money left in your budget will be returned to the state. For more information regarding impact to SSI benefits for the household, please consult https://www.ssa.gov/.
Supplemental Nutrition Assistance Program Benefits:
Your PPP monthly budget is not counted as income or as a resource for your Supplemental Nutrition Assistance Program (SNAP) benefits (formerly known as food stamps). However, wages paid to your PPP worker do count as income for their SNAP eligibility. If you are in the same household as the person providing your care, it may affect the amount of SNAP benefits for the household. You may decide to disenroll from the PPP at any time. This decision will not affect your SNAP benefits. However, any money left in your budget will be returned to the state.
Can someone assist me in putting together my monthly budget?
Yes. You are assigned a financial consultant who is employed by PPL who will assist in developing your cash management plan. Consultants serve as trainers, resource-locators and advisors while you are enrolled in the PPP. PPL will assign you a consultant that lives in your community and is familiar with the program. If requested, PPL will provide you with a consultant that is bilingual. However, consultants may at times be reassigned as new consultants are hired, consultants may move to new locations, or consultants change positions. If your consultant is reassigned, you will be notified ahead of time when possible. Your new consultant will reach out to introduce themselves.
Who can I hire?
The program gives you the ability to utilize an accredited agency or to hire anyone you are comfortable with, such as friends, relatives, or neighbors.
You do not have to use an agency, although this is still an option.
You can even use a combination of accredited agency workers and individuals you hire directly.
A person must meet all of these requirements to be a worker in self-direction:
• Be at least 18 years of age
• Able to perform all services/tasks needed by participant
• Able to provide care at the schedule requested
• Is authorized to work in the United States (I-9 Form required)
• Complete all necessary paperwork to provide care through PPP
You do not have to use an agency, although this is still an option.
You can even use a combination of accredited agency workers and individuals you hire directly.
A person must meet all of these requirements to be a worker in self-direction:
• Be at least 18 years of age
• Able to perform all services/tasks needed by participant
• Able to provide care at the schedule requested
• Is authorized to work in the United States (I-9 Form required)
• Complete all necessary paperwork to provide care through PPP
Am I allowed to hire a person who has been convicted of a crime?
You should be able to make informed decisions about the individuals you are hiring to provide services. Information about those individuals’ potential criminal records is an important part of informed decision-making. You can choose to use your monthly budget for a one-time $30 background check to be completed on a worker. If you are aware of a conviction and are comfortable with hiring the individual, it is allowed.
Can I get background checks performed on my workers?
Yes. You can request a variety of background checks on potential workers. PPL will provide you with information on the various background checks that are available and costs associated with this effort. You can choose to use your monthly budget for a one-time $30 background check to be completed on a worker.
Can a Personal Preference Participant also serve as a worker for another participant?
No. As a PPP participant, you cannot serve as a worker for another PPP participant, PCA program, or other personal care program.
What is the difference between hiring on my own or using an agency?
Hiring a person on your own may lead to a cost savings that may translate into more hours. In addition, you have the ability to work with a person you know and trust. If you chose to utilize an agency, it may cost more of your budget for services. However, agencies may have a larger pool of available workers to provide you with services.
How many assistants can I have?
You and your authorized representative are responsible for managing and supervising all workers. You may select as many as needed to be your primary assistants and designate the others as backup assistants. There is no limit to the number of assistants you may have but it must be supported by your budget.
How do I hire a family member to be my worker?
Your family member can serve as your paid worker through the Personal Preference Program. You may hire your husband, wife, or legal guardian to be your worker. You may hire a brother or sister, one of your children or grandchildren, nieces, nephews or other extended family. When you hire a family member as your worker, remember that the wages they earn will be counted as personal income if they are receiving or applying for any government benefits such as Supplemental Support Insurance (SSI) and Supplemental Nutrition Assistance Program (SNAP). It will be treated as any other job that they have.
What if I don’t know anyone to hire?
Contact us : support@HomeHealthAmericare. We are here for you
How do my workers get paid?
Your worker will fill out a timesheet that you, as the employer of record, or your authorized representative will approve. PPL provides an internet based web portal, BetterOnline™ that allows service coordinators, participants, and their families to view individual budgets, service authorizations, and spending history in real time. You will be able to submit program related forms, review timesheets, manage your cash management plan and track the payroll process. Your worker can choose to have their paycheck mailed to their home or have it directly deposited into their bank account. If you do not have access to a computer or the internet, PPL will provide you and your worker(s) with paper timesheets.
What happens if I do not spend my entire monthly budget? Can I roll the unspent funds into next month’s budget?
No, monthly budgets do not roll over. However, your financial consultant may help you identify money in your cash management plan to set aside for the purchase of approved goods and service
What happens to my participation in the Personal Preference Program during a Hospital/Rehab Facility/Nursing Home stay?
Your participation in PPP will be suspended for the time you are away from home (i.e. hospitalization, rehabilitation, nursing home, etc.). Your worker will not be allowed to work or submit timesheets during your absence from home, since the facility is responsible for meeting your daily personal care needs. You must let your MCO and PPL know whenever you are in the hospital or other facility. You will also need to notify them when you return home so you may resume your PPP services.
What happens if I go on vacation or leave New Jersey for an extended period of time?
If you are planning a vacation outside of New Jersey you must provide the dates of travel to your MCO and PPL before you travel. If you leave the state for more than 30 days, you will not remain eligible to receive PPP services and dates of service will not be paid during that time. If your dates of travel outside of New Jersey are less than 30 days, your worker may be paid for time worked within program rules
What is the role of the State Program Office in the Personal Preference Program?
The New Jersey Division of Medical Assistance and Health Services is the State Program Office that handles the administrative duties of the program. This office houses the program director and other support staff who provide quality assurance and oversight of PPL and the Managed Care Organizations. This office ensures that all state and federal rules and regulations pertaining to the PPP are being followed.
What rights do I have as a participant in the Personal Preference Program?
• You have the right to create a cash management plan that meets your individual needs and satisfies the rules and the guidelines of the program.
• You have the right to change the cash management plan to meet your needs as they change along the way.
• You have the right to be safe and be treated with courtesy, consideration, dignity and respect.
• You have the right to privacy and confidentiality. • You have the right to live as you choose, in your own home, free from judgment or interference.
• You have the right to choose an authorized representative to help you with any decisions about the program and the right to change that representative if needed.
• You have the right to file a complaint with the PPP state program office should you feel your rights are being violated by anyone in this process.
• You have the right to be informed of any/all service fees associated with the fiscal intermediary and the MCO.
• You have the right to change the cash management plan to meet your needs as they change along the way.
• You have the right to be safe and be treated with courtesy, consideration, dignity and respect.
• You have the right to privacy and confidentiality. • You have the right to live as you choose, in your own home, free from judgment or interference.
• You have the right to choose an authorized representative to help you with any decisions about the program and the right to change that representative if needed.
• You have the right to file a complaint with the PPP state program office should you feel your rights are being violated by anyone in this process.
• You have the right to be informed of any/all service fees associated with the fiscal intermediary and the MCO.
Can I pay my caregiver/worker overtime if they work more than 40 hours a week?
Generally, a single caregiver in PPP will be authorized to work no more than 40 hours in a week. There may be situations when a worker may need to work more than 40 hours per week, such as, when another caregiver is unable to be present. Working more than 40 hours per week will need to be authorized by the MCO and will be permitted under very limited circumstances as outlined in your Back-up Plan. A single caregiver working more than 40 hours by law must be paid time and a half for hours more than 40 that you must be able to afford in your budget.
To prevent the need for overtime on a regular basis, you can hire another worker for any hours that go beyond the 40 hour work week. The PPP allows and encourages you to use two workers if your care needs exceed 40 hours, with one assigned 40 hours and the other for those hours over 40. In these circumstances, both workers will be paid regular time, not time and a half. This will reduce the impact on your monthly budget, as overtime hours must be supported by your budget. Your PPL consultant can assist you in making these important decisions.
To prevent the need for overtime on a regular basis, you can hire another worker for any hours that go beyond the 40 hour work week. The PPP allows and encourages you to use two workers if your care needs exceed 40 hours, with one assigned 40 hours and the other for those hours over 40. In these circumstances, both workers will be paid regular time, not time and a half. This will reduce the impact on your monthly budget, as overtime hours must be supported by your budget. Your PPL consultant can assist you in making these important decisions.
What is the Live-In Exemption and how does it affect the requirement for overtime pay?
Some workers may qualify for a live-in exemption.
A live-in worker is exempt from the overtime requirement if the worker resides on the participant’s/employer’s premises either permanently or for an extended period of time.
• The participant/employer’s premises means the household where the worker is employed.
• Permanently or for extended periods of time means that the worker lives, works and sleeps in the household where they are employed for at least five days a week (120 hours or more).
Qualifying for the live-in exemption allows a worker to work more than 40 hours per week for a program participant at the regular hourly rate, which you must be able to afford in your budget.
A live-in worker is exempt from the overtime requirement if the worker resides on the participant’s/employer’s premises either permanently or for an extended period of time.
• The participant/employer’s premises means the household where the worker is employed.
• Permanently or for extended periods of time means that the worker lives, works and sleeps in the household where they are employed for at least five days a week (120 hours or more).
Qualifying for the live-in exemption allows a worker to work more than 40 hours per week for a program participant at the regular hourly rate, which you must be able to afford in your budget.
How does a worker qualify for Difficulty of Care?
Some workers may qualify for Difficulty of Care based on where both you and your worker live. When the worker completes an application they will be asked to respond to the following questions:
• I provide services to a participant in my (the worker’s) home
• I do not have a separate home (away from the participant) where I reside
• This is the home where I (the worker) reside and regularly perform the routines of private life, including shared meals and holidays with family.
All three of the above statements must apply in order to qualify for Difficulty of Care. Federal taxes may not be withheld if a worker qualifies for Difficulty of Care. The Difficulty of Care Federal Tax Exclusion is not optional. If a worker qualifies, he or she must complete the required paperwork
• I provide services to a participant in my (the worker’s) home
• I do not have a separate home (away from the participant) where I reside
• This is the home where I (the worker) reside and regularly perform the routines of private life, including shared meals and holidays with family.
All three of the above statements must apply in order to qualify for Difficulty of Care. Federal taxes may not be withheld if a worker qualifies for Difficulty of Care. The Difficulty of Care Federal Tax Exclusion is not optional. If a worker qualifies, he or she must complete the required paperwork
How do I apply for the Personal Preference Program?
Interested NJ FamilyCare members may contact their MCO and request options counseling or tell them they are interested in applying for the PPP to begin the enrollment process.
The MCO’s Care Managers help provide options counseling, and can complete the initial enrollment packet to be forwarded to PPL.
Contact Information for NJ FamilyCare Managed Care Organization.-
Looking for service provider ? Call us 845-688-8999 Email : support@HomeHealthAmeriCare.com
Or contact NJ Department of Human Services Personal Preference State Program Office Division of Medical Assistance and Health Services (DMAHS) P.O. Box 712 Trenton, New Jersey 08625-0712
The MCO’s Care Managers help provide options counseling, and can complete the initial enrollment packet to be forwarded to PPL.
Contact Information for NJ FamilyCare Managed Care Organization.-
Looking for service provider ? Call us 845-688-8999 Email : support@HomeHealthAmeriCare.com
Or contact NJ Department of Human Services Personal Preference State Program Office Division of Medical Assistance and Health Services (DMAHS) P.O. Box 712 Trenton, New Jersey 08625-0712
Do I Qualify?
|
For the patient you must:
|
For the caregiver:
|